Visceral Adiposity: Why Belly Fat Is A Metabolic And Longevity Risk
- David S. Klein, MD FACA FACPM

- Mar 10
- 3 min read
Introduction
Not all body fat is metabolically equal. Subcutaneous fat—the kind we can pinch—is largely inert. Visceral fat, by contrast, is biologically active, hormonally disruptive, and strongly predictive of cardiometabolic disease, cognitive decline, and reduced lifespan.
From a clinical perspective, visceral adiposity is less about appearance and far more about risk. It reflects underlying insulin resistance, chronic inflammation, and altered endocrine signaling that accelerate disease long before traditional markers become abnormal.
What Is Visceral Fat?
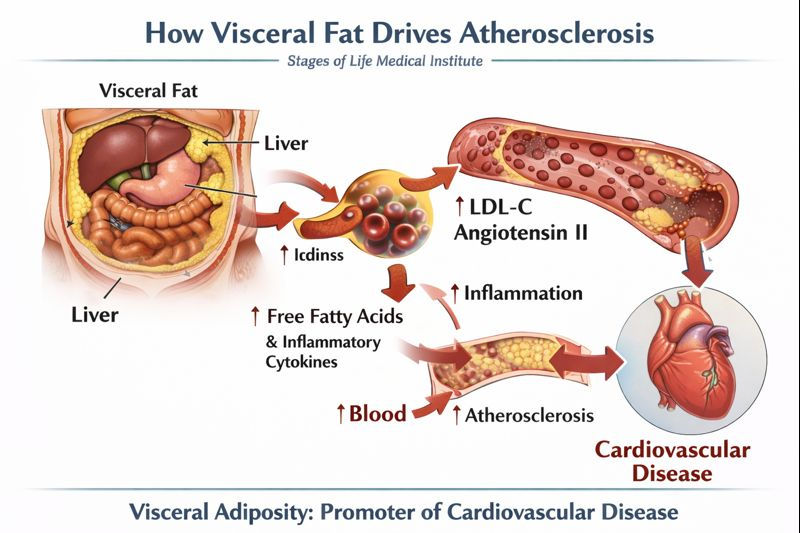
Visceral fat accumulates within the abdominal cavity, surrounding organs such as the liver, pancreas, and intestines. Unlike subcutaneous fat, visceral adipose tissue is highly vascularized and metabolically active.
It secretes pro-inflammatory cytokines, adipokines, and free fatty acids directly into the portal circulation, exposing the liver to a constant inflammatory and lipotoxic burden.
Why BMI Fails as a Risk Marker
Body mass index does not distinguish between fat compartments. Many patients with a “normal” BMI harbor significant visceral adiposity—a phenotype often referred to as TOFI (thin outside, fat inside).
Waist circumference, waist-to-height ratio, and body composition analysis provide far greater clinical insight than weight alone.

Visceral Fat and Insulin Resistance
Visceral adiposity is both a consequence and a driver of insulin resistance. Excess visceral fat:
Increases hepatic insulin resistance
Elevates fasting insulin levels
Worsens post-prandial glucose handling
Promotes dyslipidemia
This creates a self-reinforcing metabolic loop in which insulin resistance promotes fat deposition, and visceral fat further worsens insulin resistance.
Cardiovascular Consequences
Visceral fat strongly predicts:
Coronary artery disease
Hypertension
Endothelial dysfunction
Atherogenic lipid profiles
Patients with excess visceral fat often develop cardiovascular disease despite “acceptable” LDL cholesterol levels, underscoring the limitation of lipid-centric risk models.
Effects on the Brain and Cognition
Visceral adiposity is associated with reduced cerebral glucose metabolism, increased neuroinflammation, and higher dementia risk. Adipokines and inflammatory mediators derived from visceral fat cross the blood–brain barrier and impair insulin signaling within the brain.
Midlife visceral obesity is one of the strongest modifiable predictors of late-life cognitive decline.
Visceral Fat and Accelerated Aging
At a biological level, visceral adiposity contributes to multiple hallmarks of aging:
Chronic low-grade inflammation
Mitochondrial dysfunction
Hormonal disruption
Impaired autophagy
These processes accelerate vascular aging, sarcopenia, immune senescence, and metabolic fragility.

Clinical Assessment
Meaningful evaluation may include:
Waist circumference and waist-to-height ratio
Body composition analysis (DEXA or bioimpedance)
Fasting insulin and triglyceride-to-HDL ratio
Liver enzymes as a proxy for ectopic fat
Clinical Implications
Visceral fat is highly responsive to intervention. Targeted nutrition, resistance training, sleep optimization, stress reduction, and—when appropriate—pharmacologic or peptide-based strategies can substantially reduce visceral adiposity even in the absence of major weight loss.
From a longevity standpoint, reducing visceral fat is often more impactful than achieving a specific number on the scale.
Closing Perspective
Visceral adiposity is a silent but powerful driver of metabolic disease, cardiovascular risk, cognitive decline, and accelerated aging. Identifying and addressing it early allows clinicians and patients to intervene where it matters most—at the level of biology rather than appearance.
References
Després JP. Body fat distribution and risk of cardiovascular disease. Circulation. 2012;126(10):1301–1313. https://pubmed.ncbi.nlm.nih.gov/22949540/
Fox CS, et al. Visceral adipose tissue accumulation and metabolic risk. Circulation. 2007;116(1):39–48. https://pubmed.ncbi.nlm.nih.gov/17576866/
Neeland IJ, et al. Visceral adiposity and cardiometabolic risk. J Am Coll Cardiol. 2019;74(3):314–326. https://pubmed.ncbi.nlm.nih.gov/31345457/
Gastaldelli A, et al. Visceral fat and insulin resistance. Endocr Rev. 2002;23(6):725–748. https://pubmed.ncbi.nlm.nih.gov/12466187/
Kuk JL, et al. Visceral fat is an independent predictor of mortality. Am J Clin Nutr. 2006;84(2):337–344. https://pubmed.ncbi.nlm.nih.gov/16895878/
Whitmer RA, et al. Central obesity and increased dementia risk. Neurology. 2008;71(14):1057–1064. https://pubmed.ncbi.nlm.nih.gov/18367704/
Item F, Konrad D. Visceral fat and inflammation. Diabetologia. 2012;55(6):1540–1548. https://pubmed.ncbi.nlm.nih.gov/22426852/
Tchernof A, Després JP. Pathophysiology of human visceral obesity. Physiol Rev. 2013;93(1):359–404. https://pubmed.ncbi.nlm.nih.gov/23303913/
Wajchenberg BL. Subcutaneous and visceral adipose tissue. Endocr Rev. 2000;21(6):697–738. https://pubmed.ncbi.nlm.nih.gov/11133069/
Britton KA, Fox CS. Ectopic fat depots and cardiovascular disease. Circulation. 2011;124(24):e837–e841. https://pubmed.ncbi.nlm.nih.gov/22184641/
The medical references cited in this article are provided for educational purposes only and are intended to support general scientific discussion. They are not a substitute for individualized medical advice, diagnosis, or treatment. Clinical decisions should always be made in consultation with a qualified healthcare professional who can account for a patient’s unique medical history, medications, and circumstances.
1917 Boothe Circle, Suite 171
Longwood, Florida 32750
Tel: 407-679-3337
Fax: 407-678-7246








.webp)